
(Book an Appointment here or see below for information about each individual condition)
Allergic rhinitis

Allergic rhinitis, often known as hay fever, is an allergic condition that affects the nose and eyes.
It happens when the immune system reacts to allergens such as pollen, dust mites, pet dander or mould, causing inflammation inside the nose. Symptoms may occur seasonally or throughout the year depending on the trigger. Many people find their symptoms worse when pollen counts are high or during warm, windy weather. Although not dangerous, allergic rhinitis can significantly affect sleep, concentration and overall quality of life. Understanding what triggers your symptoms and managing exposure can help prevent flare-ups and improve daily comfort.
Symptoms
Allergic rhinitis (often called hay fever) and allergic conjunctivitis occur when the body reacts to allergens such as pollen, dust mites, mould, or animal dander. Symptoms usually start soon after exposure and may be seasonal or present all year round.
Nasal Symptoms commonly include sneezing, a clear runny nose, nasal congestion or blockage, and itching of the nose or throat. Symptoms may come and go or be persistent and can range from mild to more troublesome, sometimes affecting sleep, concentration, work or school.
Eye Symptoms are common and may occur alongside nasal symptoms or on their own. These include red, itchy or watery eyes, a burning or gritty sensation, and mild swelling or puffiness of the eyelids. Discharge from the eyes is usually clear and watery rather than thick or sticky. Symptoms often affect both eyes.
Some people, particularly children, may rub their nose or eyes frequently and may feel tired or irritable if symptoms are ongoing. Symptoms such as eye pain, blurred vision, sensitivity to light, facial pain, or symptoms affecting only one eye are not typical of allergic conditions and should be reviewed by your GP.
Treatment
Treatment for allergic rhinitis focuses on relieving symptoms and reducing the body’s allergic response. The most appropriate treatment will depend on the type and severity of symptoms and how often they occur.
Antihistamines are commonly used to help relieve sneezing, itching, and a runny nose. They work by blocking histamine, the chemical released during an allergic reaction. Some antihistamines act quickly to relieve symptoms, while others are taken regularly to keep symptoms under control.
Steroid Nasal Sprays are often recommended where nasal congestion or blockage is a main symptom. These work directly in the nose to reduce inflammation and swelling when used consistently.
For people with eye symptoms, such as itchy, red or watery eyes, appropriate eye drops may be recommended to soothe irritation and reduce allergic inflammation.
Treatment works best when started early, ideally at the first signs of symptoms or before known exposure to triggers such as pollen. Some people may only need treatment during certain times of the year, while others may benefit from ongoing treatment for year-round symptoms.
Cold Sores
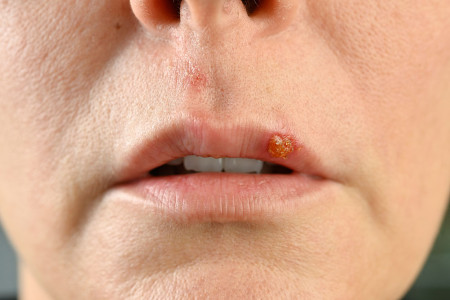
Cold Sores (Herpes Labialis) are small, fluid-filled blisters on the face, often on or near the lip and mouth, which are caused by the herpes simplex virus.
Cold sores are usually small, fluid-filled blisters around the mouth and lips that are caused by the herpes simplex virus (HSV). The virus is very common, and most individuals are exposed to the cold sore virus when they are young after close contact with someone who has a cold sore. The virus then lies dormant and from time to time, the itching and tingling around the lips indicates that an outbreak of cold sore is imminent.
Common triggers are stress, illness and or exposure to sunlight or hormonal changes. Cold sores usually heal without treatment within 10 days after the initial outbreak. The cold sore virus is spread by direct skin-to-skin contact and is highly infectious. It is important therefore, to be careful not to spread cold sores. It is particularly important to be vigilant around babies and children. Neonatal herpes can be very serious or even fatal for young babies. Their immune systems have not developed enough to fight the infection. The risk is highest in the first 4 weeks after birth.
Symptoms
Cold sores are caused by the herpes simplex virus (HSV) and usually appear on or around the lips and mouth. Many people are exposed to the virus at a young age, and it can remain dormant in the body, reappearing from time to time. They often begin with an early warning phase, where the skin feels tingly, itchy, or has a burning sensation in a small area around the lip. Within a day or two, small fluid-filled blisters may develop which can burst, weep, and then dry out to form a crust or scab. The area may feel sore while healing.
Cold sores usually heal on their own within 7 to 10 days and do not normally leave a scar, although repeated episodes in the same area may leave some skin changes over time. Some people may also notice swollen or tender glands, particularly around the neck. In children, symptoms can sometimes include sore gums, a sore throat, increased saliva, mild fever, or general discomfort.
Cold sores often recur in the same place and may be triggered by factors such as illness, stress, sunlight, or cold weather. Symptoms like severe pain, swelling, spreading infection, or sores involving the eye are not typical and you should make an immediate appointment with your GP.
Treatment
Treatment aims to reduce discomfort, shorten healing time, and help prevent the cold sore from worsening.
Antiviral creams can be used to treat cold sores and are most effective when started as early as possible, ideally at the first signs of tingling, itching, or burning. These creams help limit the activity of the virus and may reduce the duration and severity of symptoms. Treatment can still be started after blisters appear, but early use gives the best results.
Conjunctivitis
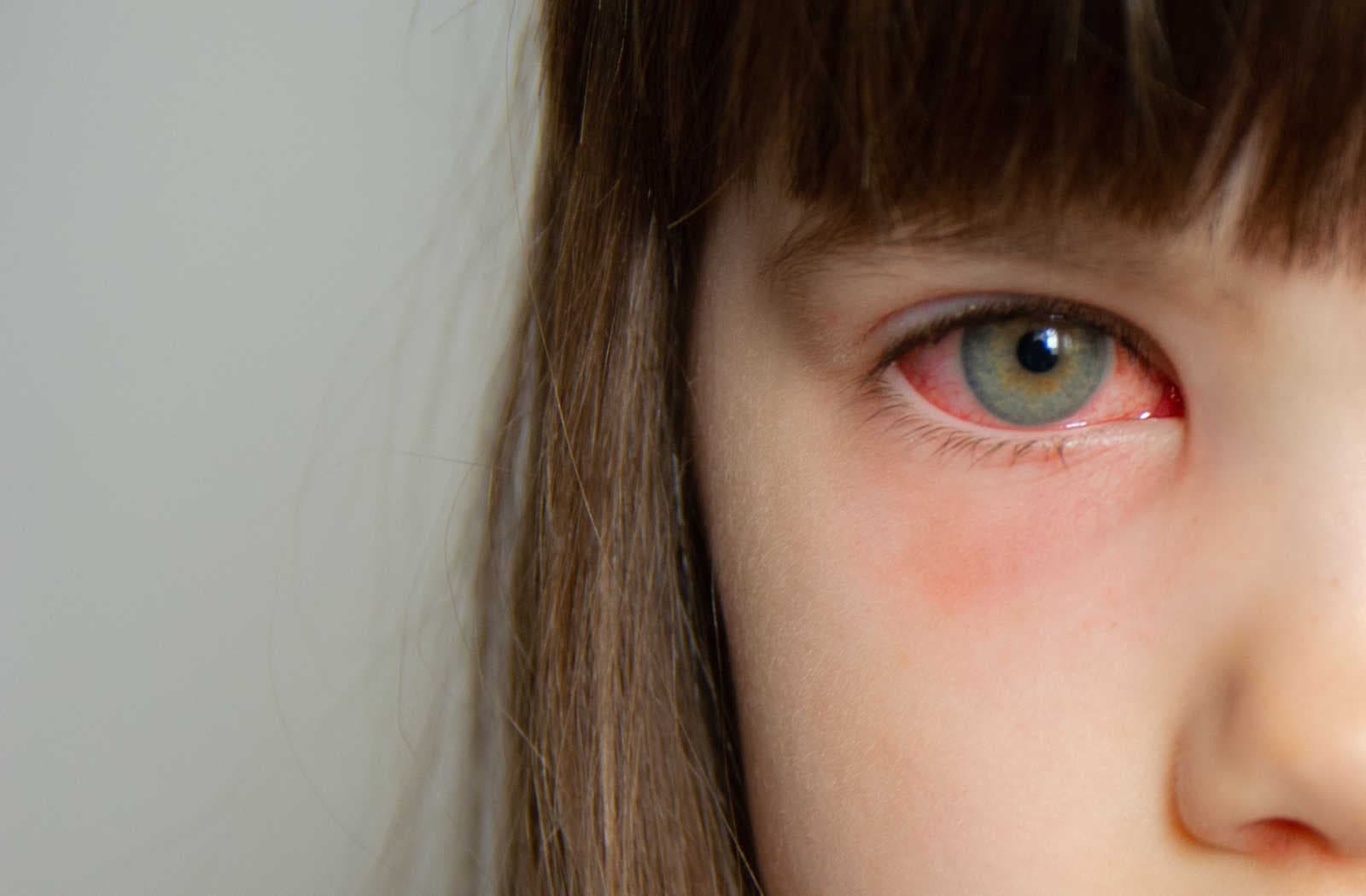
Conjunctivitis is a common eye condition which can be viral, bacterial or allergic.
Conjunctivitis is a common eye condition that causes redness, irritation and discharge from one or both eyes. It may be caused by an infection and often spreads easily through hand-to-eye contact. Most cases are mild and settle with simple treatment and good eye hygiene.
Symptoms
Conjunctivitis is inflammation or infection of the surface of the eye and inner eyelid. Symptoms can affect one or both eyes and may vary depending on the cause.
Viral conjunctivitis is the most common type. Symptoms usually include a red or pink eye, watery discharge, irritation, and a gritty or burning sensation. The eye may feel sticky on waking, and symptoms often start in one eye before spreading to the other. Viral conjunctivitis is commonly associated with cold or flu-like symptoms and is contagious.
Bacterial conjunctivitis often causes a red eye with thicker yellow or white discharge. The eye may be stuck closed on waking due to the discharge. Mild swelling of the eyelids may occur. Bacterial conjunctivitis is also contagious, but many cases are mild and self-limiting.
Allergic conjunctivitis is caused by an allergic reaction rather than infection. Symptoms usually affect both eyes and commonly include intense itching, redness, watery or stringy discharge, and mild eyelid swelling. Allergic conjunctivitis is often associated with hay fever symptoms such as sneezing or a runny nose and is not contagious.
Symptoms such as significant eye pain, sensitivity to light, changes in vision, or symptoms affecting contact lens wearers are not typical of conjunctivitis and require urgent medical assessment.
Treatment
Treatment for conjunctivitis depends on the underlying cause and the severity of symptoms. Many cases are mild and improve with simple supportive care.
Viral Conjunctivitis is the most common type and usually clears on its own within a few days to a week. Treatment focuses on relieving symptoms. Lubricating eye drops can help soothe irritation, dryness and grittiness. Cool compresses may also provide comfort. Antibiotics are not effective for viral infections.
Bacterial conjunctivitis may cause thicker yellow or white discharge. Many mild cases resolve without antibiotics. In some cases, antibiotic eye drops or ointment may be appropriate.
Allergic conjunctivitis is treated by reducing the allergic response rather than treating infection. Treatment may include appropriate eye drops to relieve itching, redness and watering, as well as managing underlying allergy symptoms. Avoiding known triggers can also help reduce flare-ups.
Regardless of the cause, treatment works best when used correctly and consistently. Our pharmacists will advise on the most appropriate option and how to use it safely.
Impetigo

Impetigo is a bacterial infection of the skin which is common in children.
There are two types of Impetigo: bullous and non-bullous. Non-bullous impetigo is the most common form of impetigo. It is usually seen around the nose and mouth. It is highly contagious until 24 hours after the person has started treatment. Lesions should be covered until crusted and healed.
Symptoms
Impetigo is a common and highly contagious bacterial skin infection, particularly in young children, but it can affect adults too. It often starts as small red patches on the skin, most commonly around the nose and mouth, but it can also appear on the arms, legs, or other areas. These patches can develop into small fluid-filled blisters which burst and form thick, golden or honey-coloured crusts.
Once the crusts dry, they leave a red mark which usually disappears within a few days or weeks, without leaving a scar. The areas are usually not painful, but they can be itchy. In some cases, especially if the infection is more severe, swollen glands or a mild fever may occur.
It is highly contagious and can spread to other parts of the body or other people. It stops being contagious 24 hours after starting using the prescribed treatment or when the patches dry out and crust over. If lesions are not yet healed after 24 hours of treatment, then they should be covered.
Treatment
Treatment depends on how widespread the infection is and the age of the person affected. Treatment usually involves a prescription for a topical antibiotic cream or ointment which is applied every 8 hours.
Before applying treatment, any crusts should be gently softened with petroleum jelly (Vaseline) and removed with a warm facecloth to help the cream work effectively. Facecloths should not be shared or reused and should be washed at a high temperature after use.
If symptoms don’t improve within 72 hours you should contact your GP.
If the infection is more extensive, involves 4 or more blisters, keeps recurring, affects very young infants, or shows signs of spreading or worsening, referral to a GP is required for further assessment and possible oral antibiotics.
Oral Thrush
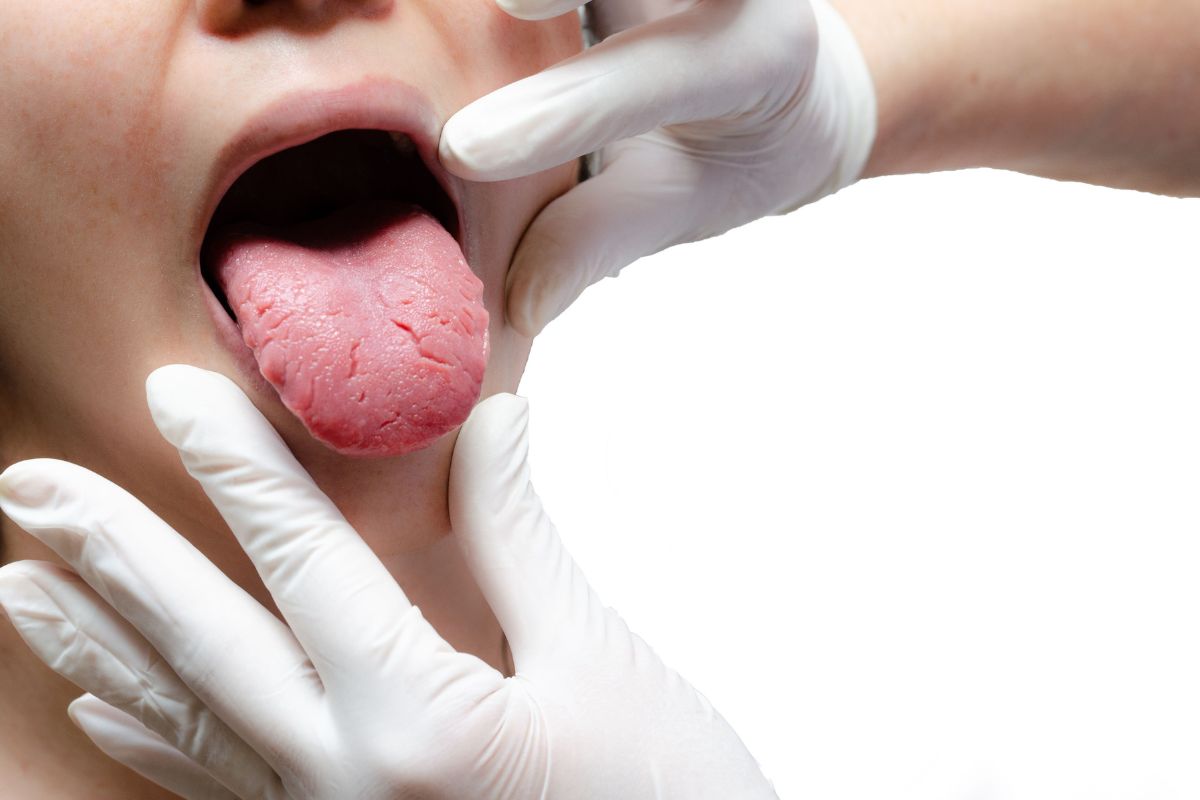
Oral Thrush is a fungal infection caused by the yeast Candida.
It is common in babies, in individuals who have taken antibiotics or steroids (inhaled or tablets), and in older people with dentures. Individuals who are immunocompromised due to underlying medical conditions or treatments may also be susceptible to this type of infection.
Symptoms
Oral thrush is a fungal infection in the mouth. It commonly causes white, creamy patches on the tongue, inside the cheeks or roof of the mouth. These patches may look like milk but do not wipe away easily, and if removed can leave the skin underneath red and sore. Some people experience a sore or burning mouth, altered taste, or discomfort when eating or drinking.
In babies, oral thrush may appear as a white coating on the tongue or inside the mouth, and the baby may be unsettled or reluctant to feed. In people who wear dentures, thrush can cause redness or soreness underneath the denture, sometimes without visible white patches.
Treatment
Treatment depends on age and symptoms. Under the Common Conditions Service our pharmacists can assess and treat adults and children aged 1 month and over with suspected oral thrush where appropriate. Treatment usually involves an antifungal liquid or gel applied inside the mouth for a number of days, and it is important to continue treatment for the full recommended course, even if symptoms improve sooner.
If symptoms do not improve, keep coming back, last longer than 14 days, or if swallowing becomes painful, referral to a GP may be required for further assessment.
For breastfed babies with oral thrush, both the baby and the mother require treatment at the same time, even if the mother has no symptoms. A topical anti-fungal treatment is available which should be applied to the nipple and areola after every feed. Any visible cream should be wiped off gently prior to the next feed.
Shingles

Shingles is caused by the reactivation of the Varicella zoster virus in people who have been previously had chickenpox.
The virus remains dormant for years before it is reactivated. The reactivated virus travels down the nerves to the skin and causes a rash. Shingles can occur at any age but is more common in older people or individuals who are immunocompromised.
Symptoms
Shingles often begins with pain, tingling, itching or burning in a specific area of the skin, usually on one side of the body. This discomfort can start a few days before any rash appears and may feel sharp, stabbing or throbbing.
A rash of small, fluid-filled blisters then develops in a band-like pattern, most commonly on the chest, back or side. The blisters burst, dry out and form scabs over several days.
The area can be very painful and sensitive to touch, and some people may also feel unwell with tiredness, headache or a mild fever. Symptoms usually improve gradually, but the rash can take several weeks to fully heal.
Treatment
Shingles is caused by a virus, and treatment works best when started as early as possible, ideally within 72 hours of the rash appearing. Under the Common Conditions Service, our pharmacists can assess and treat adults aged 18 years and over with shingles who meet specific criteria. We may be able to prescribe treatment where:
- You are within 72 hours of the rash starting, particularly if aged 50 years or over, or
- Your rash is causing moderate to severe pain, or
- Your rash affects areas such as the arms, legs or neck, or
- You are aged 70 years or over, or continue to develop new blisters.
Treatment usually involves a prescription for antiviral medicine, which helps reduce the severity and duration of symptoms and lowers the risk of ongoing nerve pain. Pain relief is also important, and simple painkillers such as paracetamol or ibuprofen may be advised by our pharmacists, if suitable.
Some people will need referral to a GP or hospital for further assessment, including those who are pregnant or breastfeeding, those with a weakened immune system, or if the rash affects the eye or face, or if symptoms are severe or worsening.
Uncomplicated UTI / Cystitis

Urinary Tract Infections are fairly common infections that affect the bladder (cystitis), the kidneys and the tubes that connect these organs.
Urinary tract infections can be painful and very uncomfortable, but they are treatable and don’t usually last more than a few days. Lower UTIs affect the bladder or urethra (the tube that carries urine out of the body). Upper UTIs are infections of the kidneys or ureters (tubes connecting the kidneys to the bladder). Both are treatable. UTI’s occur most frequently in women, but men and children can also suffer from UTI’s.
Symptoms
An uncomplicated lower urinary tract infection (often called cystitis) usually causes symptoms that come on suddenly. The most common symptoms include a burning or stinging sensation when passing urine, needing to pass urine more often than usual, and a strong or urgent need to urinate, even when little urine comes out. Some people experience lower stomach discomfort or pressure just above the pubic bone.
Urine may appear cloudy or have a strong smell. A small amount of blood in the urine can occur and visible blood should always be checked by a GP.
Importantly, symptoms of cystitis do not usually include vaginal discharge, fever, back pain, or feeling generally unwell — these symptoms may suggest a different condition and need medical review.
Treatment
Under the Common Conditions Service, our pharmacists can assess and treat non-pregnant females aged 16 to 64 years, where symptoms are consistent with an uncomplicated lower UTI.
We may be able to prescribe an antibiotic where:
- Your symptoms include burning on urination, urgency or frequency
- You have no fever, side or back pain
- You have no visible blood in the urine
- You have no vaginal discharge or change in discharge
- Your infection is not recurring
Some mild infections may improve with pain relief and fluids alone. Where antibiotic treatment is needed, our pharmacists can supply a short 3-day course of an appropriate antibiotic, selected in line with national guidance. The choice of treatment depends on symptoms, medical history and suitability.
People who are pregnant, aged 65 or over, male, immunocompromised, have diabetes, kidney disease, recurrent UTIs, or symptoms suggesting a more serious infection will be referred to a GP for assessment.
Vulvovaginal Thrush

Vulvovaginal thrush is one of the most common causes of vulvovaginal itching and discharge.
Vulvovaginal thrush is a common yeast infection caused by an overgrowth of Candida, a fungus that naturally lives harmlessly in the vagina. When the natural balance is disrupted, the fungus can multiply and lead to irritation and discomfort. This condition is very common and can affect women of any age. It may be triggered by antibiotics, hormonal changes, pregnancy, diabetes, stress, or irritation from perfumed products. Vulvovaginal thrush is not sexually transmitted and is usually harmless, but symptoms can be distressing. Although it often clears quickly with treatment, recurring episodes may indicate an underlying cause that needs attention.
Symptoms
Vulvovaginal thrush commonly causes itching and irritation around the vulva or inside the vagina, which can range from mild to severe. The area may feel sore, tender or swollen, and the skin can appear red or inflamed. Many people notice a thick, white vaginal discharge, often described as looking like cottage cheese. This discharge does not usually have a strong or unpleasant smell.
Other symptoms can include a burning or stinging sensation when passing urine, discomfort or pain during sex, and soreness or small cracks in the skin around the vulva. Some people may notice increased discomfort just before their period. Symptoms can vary from person to person and may be more noticeable at night or after exercise.
Treatment
Under the CCS, our pharmacists can assess and treat females aged 16 to 60 years, where symptoms are consistent with uncomplicated vulvovaginal thrush.
Treatment for vulvovaginal thrush usually involves a short course antifungal medicine, and both vaginal and external treatments are effective. Most people are treated with a vaginal pessary, inserted at night for one, three or six days depending on the product used. An antifungal cream may also be recommended for use on the outside of the vulva to help relieve itching, redness and soreness.
In many cases, a cream alone is not enough to fully treat thrush and is best used alongside a vaginal pessary. The choice of treatment depends on where the symptoms are located, personal preference and product availability. If symptoms include significant inflammation or irritation of the vulva, a combination cream containing an antifungal and a mild steroid may be advised for short-term use.
It is important to complete the full course of treatment. Menstrual bleeding can reduce the effectiveness of vaginal treatments, so treatment is best completed before a period starts or restarted once bleeding has eased. Some people will need referral to a GP for assessment, including those who are pregnant, have recurrent thrush, diabetes, symptoms that do not improve, or symptoms that suggest another cause such as bacterial vaginosis or a sexually transmitted infection.
